Understanding weakness: causes, signs, and what to do
Weakness is more than feeling tired. It can be a short spell after a hard day or a sign of something medical. Knowing common causes and simple steps to take helps you act fast and avoid panic.
Common causes and clues
Think about timing. Sudden weakness suggests stroke, serious infection, or a heart issue. Gradual weakness often links to anemia, low thyroid, chronic illness, medication side effects, poor nutrition, or ongoing fatigue. Muscle weakness after a workout or flu is normal. But weakness that limits daily tasks or gets worse needs attention.
Look for patterns. If weakness follows meals, low blood sugar may be to blame. If it comes with muscle cramps, check electrolytes like potassium and magnesium. If weakness arrives with weight loss, night sweats, or fever, infections or cancer should be ruled out. Mood matters too: depression and anxiety can drain energy and make muscles feel weak.
Practical steps you can take now
Start simple. Track when weakness happens, what you were doing, and any other symptoms. Note medications and supplements. Prioritize sleep, drink water, and eat a balanced meal with protein and salt if you suspect low blood pressure. Gentle movement and light strength exercises can help when weakness is chronic but not severe.
Check your medications with a doctor or pharmacist. Many drugs cause weakness as a side effect, including blood pressure meds, antidepressants, statins, and some antivirals. Stopping or changing a drug without guidance is risky. A clinician can suggest alternatives or adjust doses.
Ask for basic tests. A simple blood count, thyroid test, blood sugar, and electrolyte panel often finds the cause. For heart or nerve worries, your doctor may order ECG, imaging, or nerve studies. Physical therapy helps when weakness follows injury or prolonged bed rest.
When to get emergency help? Call emergency services for sudden weakness on one side of the body, trouble speaking, sudden severe headache, fainting, chest pain, trouble breathing, or rapid worsening. These can signal stroke, heart attack, or other life threatening problems.
Long term care may include treating the underlying condition, rehab, dietary changes, and targeted medicines. If fatigue and weakness persist despite fixes, ask for a specialist referral. Keep notes on progress and bring them to appointments.
Weakness is common and often treatable. Small changes like fixing iron deficiency, adjusting meds, or improving sleep can make a big difference. If you are unsure, reach out to a healthcare provider and share clear details. That helps get you the right tests and faster relief.
Quick checklist to bring to your appointment: a one week log of symptoms and energy levels, list of all medications and doses, recent illnesses or injuries, diet changes, and any mood swings or sleep problems. Include family history of heart disease, strokes, autoimmune disease, or neuromuscular disorders. Bring recent lab results if you have them. Clear notes save time and help your clinician focus on the most likely causes. Act early for better recovery and outcomes.
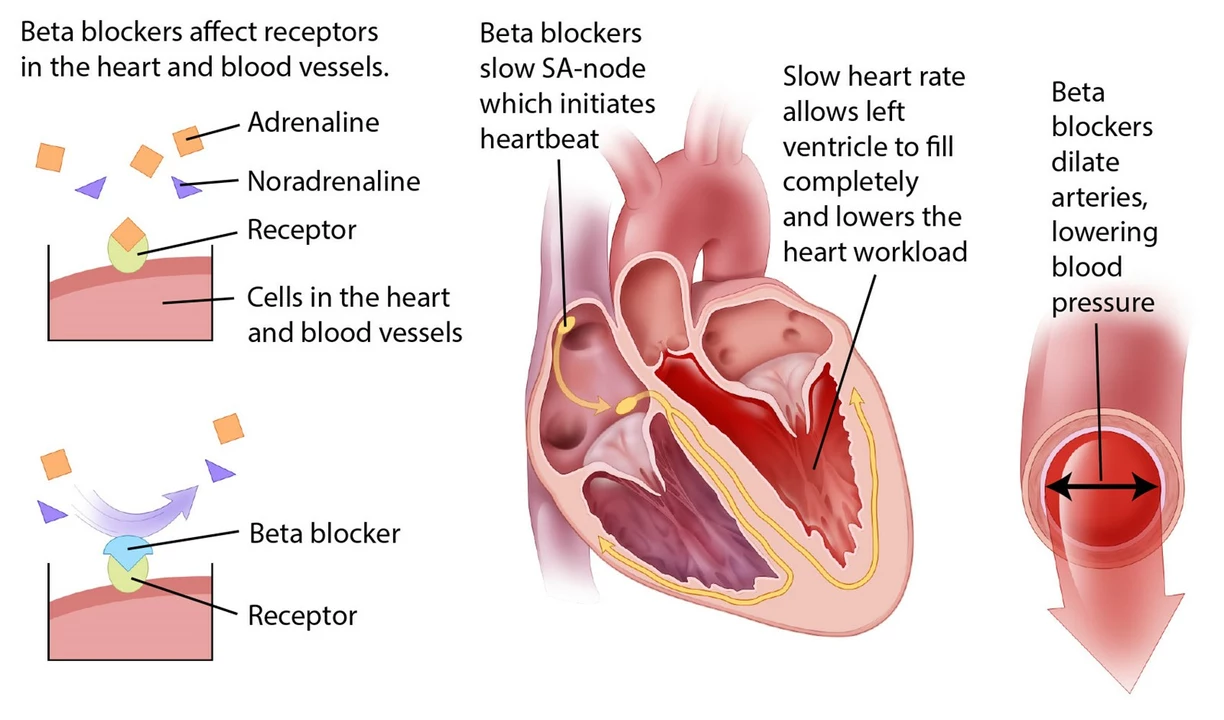
Atenolol and Weakness: Is It a Side Effect?
- 19 Comments
- Apr, 28 2023
I recently came across some information about Atenolol, a medication commonly prescribed for high blood pressure and heart issues. It seems that some users have reported experiencing weakness as a side effect. After doing some research, I've found out that weakness is indeed listed as a potential side effect of Atenolol. If you're taking this medication and experiencing weakness, it's important to discuss this with your healthcare provider. They can help determine if it's related to the medication and suggest possible alternatives or adjustments to your treatment plan.
